


What causes misses in self tests of 50% or even more? What do we know based on data from clinical practice?
In part 1, I showed that the tests can have a miss rate of 1 out of 3 to 1 out of 4 when professionals use it, and even a miss rate of 1 out of 2 when professionals use it in emergency settings. In part 2, I looked at miss rates of 50% for self-testers, and that late self-testing contributes to missing infections.
Today, I look at reason 5 and 6 that may contribute to high miss rates.
I checked the reasons against available data from the RIVM and Foundation for Innovative New Diagnostics (FIND), and a recent publication that was cited in the national news a lot.
And I give you a bonus reason: in practice, it is easy to mess up.
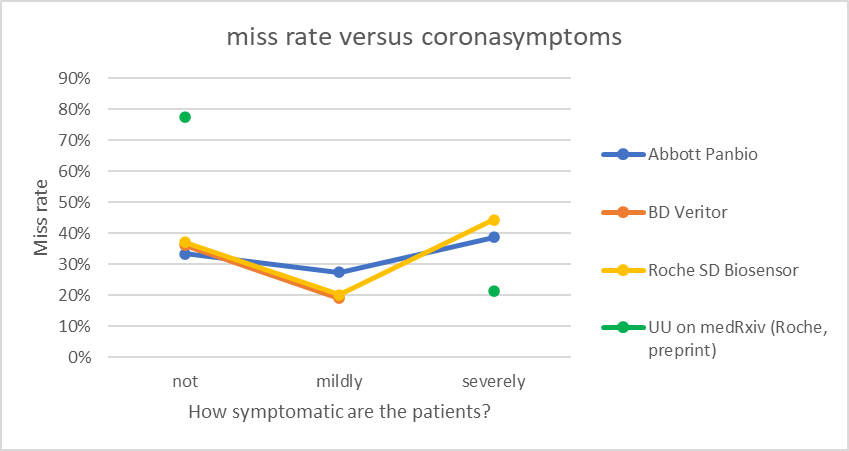
It is quite a widespread belief that antigen tests are more reliable if you’re symptomatic. But is this true? Available data on antigen tests from the RIVM (limited to data where only one variable changes), suggests that the tests are most reliable on mildly symptomatic groups. A preprint of an article written by the University of Utrecht, much cited in the Dutch press in recent weeks, suggests that there is a strong relation between symptoms and the miss rate of self-tests.
The picture, based on RIVM data and data from the University of Utrecht (UU), shows how the miss rate is related to symptom level for three different antigen tests.
Does it matter how symptomatic you are for the result to be more reliable? I believe data should be interpreted with caution, as one set of data does not show a linear relation, and the other set of data contains data on only 31 asymptomatic patients. Perhaps more variables than just the level of symptomaticity changes? Do you have other data that gives a better insight?
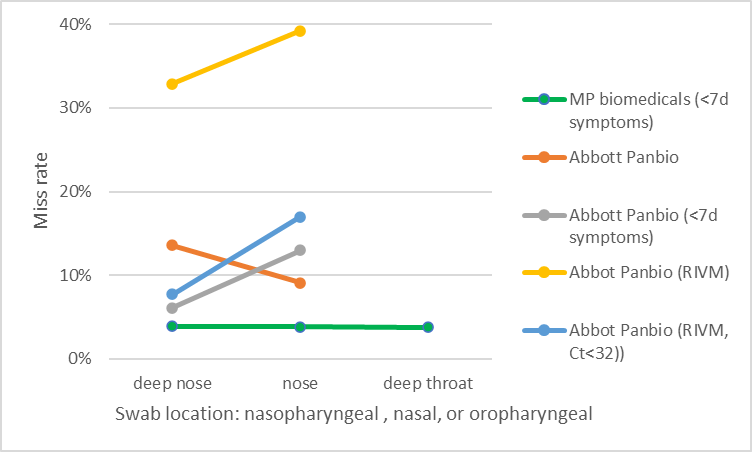
Does it matter where you collect the sample? Deep in the nose, or just 2 – 2,5 cm up your nose? The data (part IFU, part FIND, part RIVM,) so far is inconclusive and not uniform. See the picture for the miss rates and how they vary with swab site. I don’t see the correlation based on the data.

Why do half of the self-test miss a positive result? Why do self-testers score worse than pros?
Messing up the test is a real issue. Out of the first four self-tests (3 brands), I messed up two.
First mistake, first test: reading the complex instructions with one eye, and dripping sample on the read-out window instead of in the sample well.
Second mistake, fourth test: the sample well for this test was extremely small and nothing happened for a few minutes after I dripped the drops. Then I poked the sample with the swab to remove potential trapped bubbles (user mistake! contamination alert!). Then it worked.
The instructions for use are complex for lay persons, and differ per brand.
The good news: all test devices have a control-stripe “C”, that does not color when the sample does not contain enough mucus, does not reach the test strip, or the test device is too old. What happens in the other cases is not totally clear, apart from “potentially incorrect result”.
All in all, there are plenty of options to do something wrong and mess up the test, and come up with an unreliable result. Which is why it is a good idea to get the PCR test when you’re symptomatic.
If you read the instructions (IFUs) for self-tests, it seems they are reliable. However, in practice, they may miss half of the cases, and professionals using these tests also score much lower. The reasons why:
Often heard reasons that, where the data does not provide ground for a solid conclusion yet:
Whatever the reason for false negatives, just get a PCR test when in doubt. Stay healthy, stay safe!
You know of more reasons and more data? Please let us know. I’d love to hear more insights and see more data to get a better view !
Do you need help getting the right clinical data to obtain a CE mark for a SARS-COV2 (self) test under IVDR (upclassified from self-certification under IVD to the highest risk class, class D under IVDR)? Do you need with setting up a performance evaluation and/or clinical tests for any other upclassified IVD? Do you need help determining if your IVD may be part of the 80% IVDs that are upclassified? Please do not hesitate to reach out!
Ines,
Enschede, 28-DEC-2021